Designed to be unreachable
By Kinya Kaunjuga

He could no longer feel his feet.
In a way he was thankful because it also meant he couldn’t feel the coral piercing his skin, and the fish stinging him. Maybe they numbed their prey with poison before they ate it.
It was becoming obvious to Jackson Mugambi, a clinical officer at SAFARI Doctors, that Kiwayu island was designed to be unreachable.

He didn’t know what was worse, the way the box of medications was crushing his shoulders or how it was making him sink further into the knee deep muddy water.
As though his mind was intricately connected to the hope of reaching land, his legs seemed to carry him toward the shore on their own despite his total disorientation from pain and exhaustion.
He could no longer see the rest of his team but he knew they were ahead of him and he also knew many people were counting on them for treatment that day.

It was a normal work day and we were on a routine medical sail.
After completing the clinic on Mkokoni island, we packed up and set off to Kiwayu island which is on the Kenyan border with Somali.
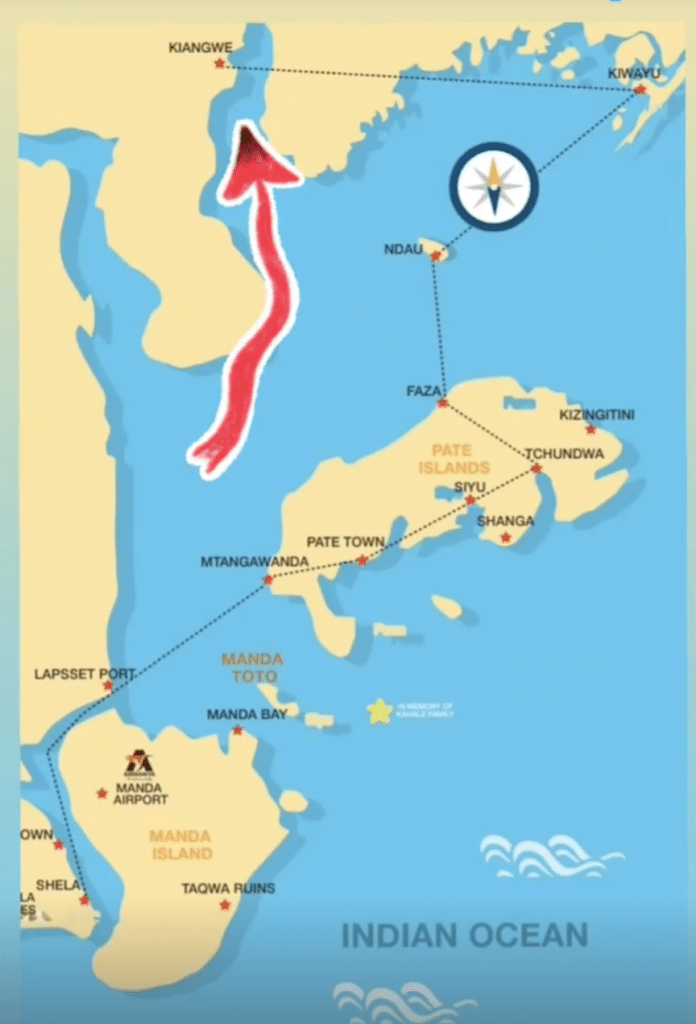
Besides being the furthest island on the east of the Lamu archipelago, we would also discover why Kiwayu was known for its high hills that framed the ocean’s horizon and its tall sand dunes with pointed peaks.
About 32 nautical miles from Mkokoni – a distance of 62km – our boat simply ground to a halt. We had gradually been sailing above cusps of sand and coral when the ocean dried up.
We could see the island about 1km away but were stuck in the boat because of a low tide.

We decided to walk. It takes months to plan a medical outreach.
Also we were keenly aware the communities living there could not afford to travel to the mainland for medical care and so they would be waiting anxiously for our clinic.

The tide can take between 4 to 5 hours to come back so we had to leave the boat in the ocean.
On foot, the fastest and strongest of us made it to the island in an hour.
Once each of us reached the island, we would treat each others cuts from the coral reef. Then as soon as everyone was stitched up and bandaged, we continued climbing the island.

We were supposed to begin the medical clinic at 9am but we started at 11am.
The islanders had waited for us and we couldn’t blame the captain. Some islands are raised so they’re very hard to reach.

Technology in caring hands can make a world of difference



“When I came to Lamu to work with SAFARI Doctors, I saw that we needed a better health management system.
We had 3 options and looked at sustainability, cost, saving time and money, and improving the care of patients by using digital data storage.
Most facilities like ours at SAFARI Doctors are poor facilities that treat the most poor people. So saving time and money is critical to sustain our operations and continue serving patients.
Our biggest wins with BandaGo are its ability to capture, store and retrieve data, and generate reports.
It used to take one whole day to complete mandatory government reports. Now, even when I am not in our facility I can tell my staff to generate the reports and forward them to the ministry of health (MOH) and it takes less than 10 minutes digitally,” says Mugambi.
$5000 helps us improve BandaGo and get it into another clinic
Thanks to you, our technology solution BandaGo continues to support the heroes who run medical clinics in slums and remote villages with an affordable yet robust health management information system.
Thanks to you, the clinics using our technology have now treated more than half a million patients as of this year, 2022!
We hope you’ll continue to help us reach our goal of treating 1 million patients in 150 clinics by the end of 2023 because you’ve made all this possible!
Photos in this article are courtesy of SAFARI Doctors, @dukprnc_creativephotos and @nyuso_za_nairobi.

Kinya Kaunjuga
Kinya brings passion, an infectious laugh and 15 years of experience in the corporate and non-profit world to Banda Health. A Texas A&M alumni with a degree in Journalism and Economics, she says, "I love doing things that matter!"

